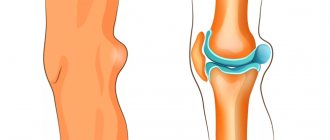
Bartholinitis is an inflammation of the large Bartholin gland. The Bartholin gland, in turn, is a paired organ that is located in the subcutaneous fatty tissue of the labia majora. When a large gland in the vestibule of the vagina becomes inflamed, microorganisms affect the excretory duct of the gland (canaliculitis), as well as the gland itself.
The main function of the Bartholin gland is to produce secretions that maintain constant moisture in the vagina. What is it for?
This secretion is released in large quantities during arousal during sexual intercourse to facilitate penile insertion. In addition, secretion is very important during childbirth. Thanks to it, the vaginal muscles stretch well and the baby can be born without damaging the vaginal walls. If the Bartholin gland does not produce secretions in the required quantity, the vagina will become dry - discomfort, itching and burning in the perineum and pain during sexual intercourse will appear. Normally, this is only possible during menopause due to the age-related decrease in female estrogen hormones.
Causes of bartholinitis:
Bartholinitis occurs due to infection in the Bartholin gland through a narrow opening of the excretory duct on the inner surface of the labia minora. Once deep into the gland, microorganisms actively multiply. This leads to inflammation and suppuration of the Bartholin gland.
Not all genitourinary infections cause bartholinitis. In the vast majority of cases, bartholinitis is provoked by sexually transmitted infections. Most often it is gonorrhea, less often - trichomoniasis and chlamydia.
Bartholinitis of nonspecific etiology is extremely rare - in this case, the causative agent is bacteria - staphylococci, Escherichia coli, streptococci, and so on. This is possible if personal hygiene rules are not followed. It should also be taken into account that even in the presence of sexually transmitted infections, bartholinitis does not develop in everyone and not always.
Immunity plays an important role in the development of the disease: if it is weakened, the chances of developing bartholinitis increase.
Depending on the clinical course of the disease, bartholinitis can be acute or chronic. Acute bartholinitis is characterized by the formation of a true or false abscess of the Bartholin gland (a limited focus with pus).
When a false abscess forms, the excretory duct of the gland first becomes inflamed (“canaliculitis”, in scientific terms). The skin over the site of inflammation turns red and swells. If you press on the inflamed area, pus will come out. Next, a blockage of the excretory duct of the gland occurs and pus is no longer released, but accumulates in the Bartholin gland. Because of this, the gland is greatly stretched and protrudes, forming a painful “bump”-shaped formation. During movements - when walking, running, during sexual intercourse - the pain intensifies, and a burning sensation appears in the perineum. Sometimes body temperature rises slightly. If you do not contact a gynecologist for a long time, the disease becomes chronic.
With a true abscess, the infection penetrates directly into the Bartholin gland, and the parenchyma of the gland melts. In this case, the symptoms of the disease are more pronounced than with a false abscess. The labia majora and minora become very swollen. The body temperature rises to more than 38 degrees, the inguinal lymph nodes enlarge, chills, weakness, and “pulsating” sharp pain in the labia majora appear. Spontaneous opening of the abscess with the release of yellow-green pus is possible, which leads to a weakening of the symptoms of the disease. But if left untreated, the inflammation recurs again and gives complications, or, like a false abscess, becomes chronic.
In the chronic form of bartholinitis, the symptoms of the disease temporarily subside and worsen again. Instead of an abscess, a cyst (liquid formation with inflammatory exudate) forms in the gland.
With any form of bartholinitis, you should never self-medicate or try to squeeze out an abscess or cyst - this can lead to blood poisoning . If such symptoms occur, you should immediately consult a gynecologist.
Pathogenesis
The resulting inflammation of surrounding tissues occurs in 3 stages:
Stage 1 - Alteration the release of fluid during Stage 2 - Exudation and blood cells from the vessels into the tissue, edema occurs.
Stage 3 - Proliferation (or productive stage) does not occur, since damaging factors continue to operate and therefore the resulting swelling, thickening of the walls, narrowing of the lumen of the canal, thickening of the secretion, resulting in blockage of the duct), the secretion of the Bartholin gland being produced, accumulating, thickening, leads to the formation of a cystic cavity formation, gradually increasing in size. Local defenses fail due to concomitant diseases, decreased general immunity and the aggressiveness of the flora that causes inflammation. Reaching a size of 4 or more centimeters, squeezing the surrounding tissues, causes pain in a woman and can, turning into an inflammatory process, cause an abscess of the Bartholin gland [2] [3] [4]
The causes and mechanism of development of Bartholin’s gland abscess are described below in the “Complication” section.
Diagnosis of bartholinitis:
Diagnosing bartholinitis is not particularly difficult. The doctor will be able to make a diagnosis during examination at the first appointment. In the presence of an abscess, swelling and redness of the Bartholin gland is determined; palpation of the formation causes sharp pain. In the chronic form of bartholinitis (in the presence of a Bartholin gland cyst), a tumor-like formation is detected, painless on palpation. In addition to the examination, the following tests must be taken:
- a regular vaginal smear;
- PCR diagnosis of major sexually transmitted infections (chlamydia, gonorrhea, trichomoniasis, mycoplasmosis, ureaplasmosis, herpes, human papillomavirus);
- bacteriological culture of vaginal discharge to establish sensitivity to anitibiotics;
- bacteriological examination of pus when an abscess ruptures (or the secretion can be obtained from the excretory duct of the gland by light pressure).
Differential diagnosis
Includes cystic and solid lesions of the vulva, such as epidermal inclusion cyst, hidradenoma papilliferum and lipoma [3], vulvar neoplasms; - abscess of the Bartholin gland; - bartholinitis; vulvar abscess.
— Hematoma in the vulva area – there may also be complaints about a formation in the vulva area, discomfort during sexual intercourse, and pain. But when collecting anamnesis; and gynecological examination - the woman associates its appearance with mechanical trauma, childbirth; And the location is not in the area of projection of the large vestibular gland. [1]
— Paraurethral cysts – similar complaints. On examination - swelling in the paraurethral region (the area near the urethra) [1]
- Furunculosis of the labia majora. Complaints include formations in the perineal area, general malaise, hyperemia, edema, hyperthermia. Upon examination, the formation is localized in the area of the hair follicle and sebaceous gland. [1]
Surgical treatment of Bartholin gland cyst:
Treatment of Bartholin gland cysts is carried out without exacerbation of the inflammatory process. In this case, there are two options for surgical intervention: marsupialization of the cyst (creation of an artificial duct of the gland for the outflow of secretions) or extirpation (removal) of the Bartholin gland.
When performing marsupilization, the doctor opens the cyst capsule with a linear incision. The edges of the capsule are sutured with separate sutures to the edges of the skin wound, forming an external opening. A drainage tube or catheter is inserted to drain the contents of the cyst. After the operation, within two months, the external opening narrows, and a new excretory duct is formed.
Extirpation of the gland is carried out in case of recurrence of bartholinitis. To do this, a longitudinal incision is made on the inside of the labia minora. The gland is carefully isolated with a scalpel and removed, and catgut sutures are placed on the wound.
For any types of bartholinitis, after surgery and complete elimination of the inflammatory process, physiotherapy is prescribed on the 3-4th day - magnetic therapy and ultraviolet irradiation. All patients are advised to abstain from sexual intercourse until complete recovery, since there is a high probability of infection of the sexual partner. In order to prevent a relapse of bartholinitis, it is important to eliminate the cause of the disease, to completely recover from concomitant infections (chlamydia, gonorrhea, etc.), otherwise bartholinitis may occur again.
All patients must observe the following rules of personal hygiene:
- wash your face twice a day;
- wear comfortable underwear, preferably cotton;
- During menstruation, change pads and tampons every 3-4 hours to avoid re-infection.
During the recovery period, it is important to use drugs that enhance the immune system. These include vitamins, a balanced diet, and some herbal immunomodulators.
Treatment
The choice of treatment method for bartholinitis depends on the stage of development of the disease and is determined at an appointment with a gynecologist.
Conservative treatment. In the absence of an acute inflammatory process, preference is given to conservative therapy (anti-inflammatory, antibacterial). Vishnevsky ointment, levomekol, miramistin, etc. can be used locally. This treatment of bartholinitis without surgery can be carried out at home. How exactly to treat, what antibiotics to take and for how many days, what local treatment to carry out is determined during a consultation with a gynecologist.
Surgical treatment. If the disease progresses to the stage of formation of a cyst or abscess, surgical treatment is necessary (marsupialization, installation of a word catheter).
In the case of the development of a true abscess, surgical treatment of bartholinitis is performed - an operation to open the abscess. After the operation, the wound is washed with an antiseptic solution, the cavity is drained with a word catheter to drain the inflammatory exudate. Dressings are done daily. A course of treatment for bartholinitis with antibiotics is prescribed to reduce the risk of it becoming chronic.
The Bartholin gland cyst (chronic bartholinitis) is opened using a special technique, creating a wide outlet (marsupialization), or it is completely removed (husking) along with the capsule. The operation is performed outside of exacerbation.
If you consult a doctor in the early stages, bartholinitis can be successfully treated with conservative methods. If you experience discomfort in the labia area, immediately make an appointment with a gynecologist. Don't take things to the point of surgery.
Prevention of bartholinitis:
- regular visits to the gynecologist;
- protection against sexually transmitted infections - use of condoms, monogamous lifestyle;
- timely treatment of infections;
- strengthening the immune system: good nutrition, exercise, giving up bad habits.
In our clinic you can receive a full range of clinical and laboratory examinations before performing this surgical operation. The equipped operating room allows you to perform the operation both under local anesthesia and general anesthesia, with stay and observation in the ward for several hours.
Expert advice
Bartholinitis is a disease that can have dangerous consequences. Even a small abscess creates a risk of purulent contents escaping and rupturing the gland. The result is sepsis, requiring immediate medical intervention.
If the inflammation is not treated, bartholinitis leads to the formation of fistulas and cysts. In the future, it may be necessary to remove the Bartholin gland cyst, which will negatively affect the condition of the woman’s reproductive system.
The danger is not only acute, but also chronic bartholinitis. If not treated promptly, the infection can spread to other organs of the reproductive and genitourinary system. Among the most common complications are vulvitis, adnexitis, colpitis, and infertility.
Contact your doctor at the first sign of discomfort.
Bani Odekh Elena Yurievna
Obstetrician-gynecologist, gynecologist-endocrinologist, ultrasound diagnostics doctor, Candidate of Medical Sciences Experience 23 years
We get rid of it forever
In the initial stages, bed rest is recommended, analgesic and antibacterial therapy is carried out; If the condition of the Bartholin gland cyst worsens or suppurates, surgical treatment is necessary. There are several anti-relapse surgical techniques for treating cysts. One of them is removal of the cyst; the operation can only be performed in the “cold” period, that is, until the cyst has festered. This operation is classified as a complex gynecological operation; heavy bleeding may occur during it. The least traumatic is marsupilization of a Bartholin gland cyst. The essence of this operation is that a new hole is created - the entrance to the Bartholin's gland. If this hole remains, the cyst will not form again. Complications after such surgical intervention are much less, the relapse rate is 1-2%. In our Center, both operations are performed under intravenous anesthesia. Patients are hospitalized, as a rule, for a day, then discharged home with doctor’s recommendations for postoperative treatment. The next follow-up visit to the gynecologist is in a week. If bartholinitis is detected, sexual life is contraindicated for patients due to possible infection of the partner or suppuration of the gland. Prevention of the disease consists of observing the rules of personal hygiene, excluding casual sexual intercourse, and treating vulvitis, colpitis, and urethritis.
Contraindications
Drainage of the cavity should also be carried out in case of independent breakthrough of the abscess. If this happens, you should immediately go to the hospital, as purulent contents remain in the cavity, which can cause a relapse. The doctor installs special tubes to drain the remaining fluid, after which they are treated with an antiseptic.
In addition, the contents of the abscess can enter the bloodstream and cause sepsis. For this reason, you should never open an abscess yourself or ignore the symptoms.
Be careful - strangers are in the body!
Inflammation of the female genital organs is quite easy to suspect. Sudden pain in the lower abdomen, menstrual cycle disorder, itching and strange (in color and smell) vaginal discharge - all this indicates the presence of inflammation. If, in addition, the temperature rises and weakness appears, most likely the inflammatory process is in the acute phase. Pathogenic microorganisms can enter the female genital organs in two ways: through the blood and through the vagina, and the latter route is much shorter than the first. After all, the internal genital organs of a woman are an open system by nature; it communicates with the environment through the vagina and cervix. An inflammatory disease can be caused by sex without a condom, trauma to the genital organs of any origin, failure to comply with personal hygiene rules, abortion and childbirth. When the infection circulates in the blood, for example, with influenza and scarlet fever, it can also reach the female genital organs. A similar situation is observed when somewhere in the body there is already a focus of inflammation: caries, chronic sinusitis, tonsillitis, etc. A dormant infection can “wake up” at any moment, “swim” through the bloodstream to the genitals and “arrange” inflammation. It is impossible to talk about all inflammatory diseases of the female genital organs in one article; we will focus on one of them - bartholinitis.