Cleft palate in children is a congenital malformation in which a child is born with damage in the facial area: there is a direct connection between his mouth and nose due to the fact that there is a cleft in the palate. Often this defect is combined with a cleft lip - they have a common development mechanism. If the lip is not damaged, but only part of the palate (soft palate or uvula) is damaged, or the cleft occupies its entire length, then the disease goes unnoticed for some time until the parents pay attention to strange behavior during feeding.
Cleft palate without cleft lip is observed in approximately 1-2 cases per 1000 newborns, girls are more often affected (isolated cleft lip is more common in boys). This disease leads to various complications from both the ENT organs and many internal organs, so it must be treated. Only surgery will help, the first stage of which can be performed before the age of one year. After surgery, long-term restorative complex therapy is needed.
Causes of the disease
A cleft palate, or, as it is correct and harmless for such people to say, a congenital cleft palate, occurs when the normal fusion of facial bones is disrupted in a developing fetus (2-11 weeks of pregnancy). This malformation, occurring alone or in combination with a cleft lip, is one of the ten most common defects. Children with Asian and Latin American “roots” are most often affected.
The reasons why a cleft palate appears are varied. This:
- Defective genes. The main “culprit” is considered to be the TBX-22 gene, but scientists also say that other parts of the DNA molecule can also cause cleft palate: the MSX1 and MSX2 genes, TCOF, VAX1, NOG and many others. The probability of transmitting such a gene from one of the parents is only 7%.
- Insufficient oxygen supply to the tissues of the developing fetus. This happens if the mother has not stopped smoking, drinking alcohol, or continues a course of medications that lower blood pressure, which are not allowed during pregnancy (and this is not difficult, because usually not every woman realizes that she is pregnant 2-6 weeks after conception). Also, fetal hypoxia will occur if the pregnant woman suffers from anemia, cardiovascular diseases, or if she has developed severe toxicosis.
- Chemical factors:
- working with pesticides;
- lead exposure;
- petrol;
- nitric oxide;
- herbicides;
- defoliants;
- insecticides based on organophosphorus compounds (for example, Dichlorvos);
- epoxides;
- arsenic.
- Biological factors are diseases that appeared or worsened in the first trimester of pregnancy. Acute viral, bacterial and infections caused by protozoa are especially dangerous:
- rubella;
- cytomegalovirus;
- measles;
- herpes simplex virus;
- toxoplasmosis;
- malaria;
- chicken pox;
- parotitis.
- Mental trauma, stress.
- Impacts to the lower abdomen, operations on the lower abdomen.
- Taking medications that can cause fetal deformities (that is, have a teratogenic effect):
- sodium compounds;
- anticonvulsants;
- anticancer drug "Metrotrexate";
- anti-acne drugs based on vitamin A derivatives (“Roaccutane”, “Acnecutane”);
- synthetic hormones of the adrenal cortex;
- tranquilizer "Diazepam" (also called "Sibazon", "Relanium", "Valium").
- An unbalanced diet with insufficient intake of folic acid, which is found in greens and fruits, zinc, copper or manganese.
- Obesity.
- Age over 35 years.
- Increased body temperature: due to infectious diseases, overheating in the sun, in a sauna or bath, working in a hot shop or in a laundry.
- Vibration in a factory where a woman works.
- Uterine fibroids, the node of which puts pressure on the developing fetus.
- Substances used by a woman to try to induce a spontaneous miscarriage.
- Little and polyhydramnios.
- Exposure of a pregnant woman to ionizing radiation (for example, for cancer treatment, or if she works at a nuclear power plant), X-ray radiation, UHF and microwave currents.
- Hypervitaminosis A in combination with an increase in the level of adrenal hormones in the blood (for example, with high levels of male sex hormones, which causes acne, and treatment of acne with vitamin A-based drugs).
- A long time from ovulation until the fusion of the egg with the sperm.
- In 25% of cases, the cause of cleft palate remains unclear.
Not always cleft palate with or without cleft lip. Often this facial defect is only one of a “set” of the following syndromes:
- Van der Woude - when a child is born with a cleft lip and cleft palate, pits on one or two lips;
- Stickler: in addition to cleft palates and lips, there is myopia and damage to the joints;
- Lois-Dietz - with a combination of cleft palate, lip, uvula with a large distance between the eyes and aortic aneurysm;
- Hardikar: cleft lip, palate plus hydronephrosis and intestinal obstruction;
- Patau - when cells have three thirteenth chromosomes. The syndrome is characterized by a large number of developmental defects (impaired development of parts of the brain, heart defects and internal organs), due to which most infants die in the first weeks and months of life.
However, scientists believe that the influence of genetic causes is only 10-15%. The rest is due to external influences on a pregnant woman, listed above.
For a cleft palate to occur, one or more of these factors must occur during the period from 2 to 11 weeks of intrauterine life of the fetus, just when the formation of facial structures occurs. Namely, during this period, the woman does not suspect that she is pregnant and does not limit her intake of medications, alcohol, or continues to smoke.
How does the face form?
After the egg has merged with the male gamete, its division begins. At first, the resulting cells are identical, but from the 2nd week of intrauterine development the embryo becomes two- and then three-layered, and each of these layers differs in structure and function: from one layer skin and hair are formed in each area, from the other - internal organs, from the third – bones, muscles, blood vessels in each area. And at the 4th week of intrauterine development, in the area of the head, where the brain is already beginning to develop, 5 protrusions of all three layers appear: an unpaired frontal tubercle, 2 maxillary and 2 mandibular. They move towards each other:
- the maxillary processes go towards each other, but do not connect with each other: the gap between them is filled by a process of the frontal tubercle, which grows downward. With the help of this area and the maxillary tubercles, the outer part of the nose is formed;
- mandibular - to each other: this is how the lower jaw and lower lip are formed;
- The maxillary and mandibular processes, growing laterally and connecting with each other, form the cheeks, the lateral part of the upper jaw and lips.
The outer layer forms the skin of the face, oral mucosa, tooth enamel, and glands that produce saliva. The middle layer becomes the ancestor of the facial bones, facial muscles, as well as the parts of the tooth located under the enamel.
At 7 weeks, the nose is separated from the mouth by the “primary palate”, from which parts of the upper lip, teeth and the anterior part of the hard palate are still formed. But from the 7th week, a “secondary palate” is formed - from the palatine processes that grow from the inside of the maxillary tubercles. At first they grow vertically, but when the emerging tongue moves down, the palate begins to grow horizontally and its parts are connected to each other.
The process of facial formation ends by the 11th week of life. If the connection of the embryonic processes is disrupted, facial clefts appear. This can happen in any one place, or simultaneously in several or even all of them. For example, a cleft palate is formed if the processes of the maxillary and frontal tubercle do not come together. And if the maxillary and mandibular processes do not fuse, a pathologically large mouth is formed. To do this, it is necessary that any (or several) of the teratogenic factors act at 2-11 weeks of the child’s development (especially if there is a hereditary predisposition). 3-6 weeks of life are considered especially dangerous.
Features of the structure and development of the sky
The upper palate acts as a barrier separating the nasal cavity from the oral cavity. During evolution, the sky began to form in organisms whose habitat became land. It consists of 2 parts: the hard and soft palate. The anterior part of the oral cavity is occupied by the hard palate, consisting of bone tissue, as well as the palatine processes of the upper jaw, and the horizontal plates of the bones of the palate. Immediately behind it is the soft palate, consisting of muscle tissue, aponeurosis and glands. With the help of muscles, the soft palate can change its position when pronouncing sounds or eating. The tissues of the palate prevent fluid and food from entering the upper respiratory tract. In the middle of the posterior edge is the uvula of the soft palate.
At the 8th week of fetal development, the upper jaw begins to form, consisting of 2 bones fused together. First, the formation of the palatine processes occurs, consisting of the inner surface of the jaw. As they develop, they fuse with each other and with the nasal septum, thus forming the hard palate.
Due to the presence of gene defects during the development of the maxillofacial system, the palate and upper lip do not fuse. You can find out about the development of this pathology in a child only in the last weeks of pregnancy during an ultrasound.
People with this defect constantly get sick because the air entering their lungs is not heated or moistened. They may experience various changes in the maxillofacial skeleton and hearing aid. Cleft lip and palate can be an independent disease or accompanied by the presence of other anomalies.
Classification of the disease
A cleft palate can be:
| View | What does it mean | Image |
| Hidden | Only the muscles of the soft palate are split, the mucous membrane is intact | |
| Incomplete | Only the soft palate and partially the hard palate are cleft | |
| Full | The cleft is noted on both the hard and soft palates - up to the incisive foramen | |
| Through | Both the soft and hard palates are split, as well as the area of the upper jaw where the teeth grow. Can be one- or two-sided |
Symptoms of a cleft palate
If a child's cleft palate affects only the soft palate and is not accompanied by a cleft lip, the disease is not immediately diagnosed. You can only pay attention to the fact that the child eats somehow strangely: he quickly gets tired of sucking, periodically takes breaks, and may refuse to eat.
If the cleft is incomplete, parents will know about it from the first minutes of the baby’s life: he is breathing heavily, sucking is short-lived, he chokes, and milk comes out of the nose. With a complete or through cleft, it is visible from the first glance at the child, his breathing is difficult, and sucking is impossible. Such a child may end up in intensive care immediately after birth, which is associated with amniotic fluid entering the respiratory tract.
Consequences of deformation
This pathology in children causes great difficulties and discomfort literally from the first day of their birth.
The consequences of the disease affect literally all areas of the life of the child and his family:
- At the time of birth, there is a high probability of aspiration of amniotic fluid into the baby's lungs. The process of air penetration into the body of a newborn baby is difficult, and it is difficult for him to suckle. Therefore, children with palate deformation often have less weight than their peers and are developmentally delayed.
- Before surgical intervention to correct this pathology, the child is most often fed using spoons, bottles and other specific utensils specially created for this purpose.
- Also, cleft palate and lip often lead to malfunction of the upper respiratory tract, digestive system, and to retardation or inhibition in the development of hearing and speech.
All these inconveniences and deviations in the normal functioning of the whole organism most often lead to the fact that children with such pathologies have an insufficient quality of life, and often, if the problem was not resolved in a timely manner, they feel inferior, have low self-esteem and, as a result, often There are asocial, aggressive, unsuccessful people.
Symptomatic manifestations
Children who have this pathology face the following difficulties due to a disrupted natural process:
- incorrect pronunciation and formation of sounds:
- difficulties in mastering the functioning of the speech apparatus as a whole,
- development of rhinolalia.
Rhinolalia is characterized by a change in the timbre of the voice and the nature of the pronunciation of sounds. This occurs due to improper closure of the pharynx and palate.
On top of this, inhaled air can carry food and drinks into the nose and back through the nose and into the mouth. Fluid can also enter the Eustachian tube, which sometimes causes otitis media and sinusitis. In addition, in this case, deformation of the bite and teeth occurs, which disrupts the process of chewing food.
How dangerous is a cleft palate?
Children with cleft palates are painful because the air they inhale passes into the oral cavity, where there are no systems for moistening and warming it. This leads to frequent occurrence of diseases of the respiratory tract and inner ear.
Deformation of the palate also causes speech impairment: the sound produced by vibration of the vocal cords penetrates not only the mouth, but also the nose, acquiring a nasal tone.
Otitis often occurs due to the fact that fluid and food enter the auditory tubes through the cleft palate. Due to chronic inflammation of the ear, hearing deteriorates until it is completely lost. There is a way out - this is the installation of drainage tubes on the eardrum, through which the liquid will be released out and not stagnate.
Fluid can also get into the sinuses, which leads to the development of sinusitis.
Due to a defect in the palate, sucking is difficult. As a result, the child does not receive enough nutrients and fluids, which leads to a delay in his physical (to a greater extent) and mental (to a lesser extent) development. Subsequently, tooth deformation and malocclusion complicate the chewing process, which aggravates the situation and leads to the development of diseases of the internal organs. This requires the use of special feeding devices, or the installation of a temporary “artificial palate” - an obturator.
Problems also arise directly with the teeth: they are often affected by caries.
Cleft palate, uncorrected in early childhood, leads to the development of socio-psychological problems in the child - those related to appearance. This affects the development of self-esteem, behavior and social skills. This is especially true for girls, even small girls aged 3-5 years. According to interviews with these children, they felt sad, angry, afraid, or alienated from their peers. During adolescence, boys become aggressive and experience anxiety or depression. Social life also suffers for girls, who become withdrawn and can make many mistakes in relation to the opposite sex.
What diseases do oral and maxillofacial surgeons treat?
It would be a mistake to assume that maxillofacial surgery today is limited only to the correction of congenital malformations of the face. The range of problems solved within the framework of maxillofacial surgery is quite wide.
- Firstly,
inflammatory diseases of the maxillofacial area: abscesses, phlegmon, osteomyelitis of the jaws. - Secondly,
odontogenic and non-odontogenic benign neoplasms of the bones of the facial skeleton and soft tissues of the face (papillomas, fibromas, lipomas, etc.). - Thirdly,
all kinds of defects and disorders of the formation of the dental system and bite.
A special problem in pediatric maxillofacial surgery is the elimination of the consequences of childhood injuries, the sad statistics of which are only growing over the years in all regions of Russia.
What are the most common maxillofacial injuries in children?
Injuries to children in the maxillofacial area can be roughly divided by periods of their lives.
At first, the baby is completely dependent on the parents and can only be injured due to their oversight (for example, falling out of the cradle). Then the child expands his living space: he begins to walk. Therefore, closer to the age of one year, the most common injuries to the soft tissues of the face are due to a fall from one’s own height. By the age of one and a half years, children begin to run, they are actively teething, and as a result of falls or other injuries, damage to soft tissues can already be accompanied by dental injuries of varying severity.
Then a child of 3–4 years old begins to ride a scooter and bicycle, which is fraught with fractures of the bones of the axial and facial skeleton.
Schoolchildren not only often get injured at home, but also become victims of careless handling of pets: cats and dogs, unfortunately, often bite in the nose and mouth. This leads to quite pronounced and extensive defects, and subsequently to deformations of soft tissues, the elimination of which sometimes requires multi-stage plastic surgeries with transplantation of soft and integumentary tissues.
And finally, teenagers between 15 and 18 years of age are more likely to get into road accidents, man-made disasters, come into contact with firearms and explosives, and we have to observe the tragic consequences of severe combined and combined injuries.
Yuri Olegovich Volkov
maxillofacial surgeon, candidate of medical sciences, head of the department of maxillofacial surgery of the Children's City Clinical Hospital named after. G.N. Speransky in Moscow
Diagnostics
The presence of a cleft palate can be determined in the prenatal period, but at such a stage of pregnancy (16-24 weeks) when abortion can be performed only according to strict indications, for example, if, in addition to a cleft palate, there are other developmental defects that are dangerous or incompatible with the life of the fetus (this established by a specially assembled council). In addition, not a single sonologist (one who performs ultrasound), even when examining the palate in Doppler mode, can vouch for the accuracy of the diagnosis of cleft palate. This diagnosis is established only after the birth of the child - based on an examination of the oral cavity.
If this couple has already given birth to a child with a cleft palate or lip, it is recommended that they seek medical genetic counseling before planning the next pregnancy.
Treatment
The only treatment for cleft palate is surgery. But up to a year, it can be performed only if there is a defect only in the soft palate (the operation is called veloplasty): suturing the hard palate will entail stopping its development, as a result, deformations of the skull will develop.
In any case, before surgery, the child needs to be prepared so that he can gain weight, get nutrients, and not get sick. To do this you need to go through several stages.
Preoperative preparation
It consists in:
- psychotherapeutic assistance to the child’s parents;
- organizing proper feeding;
- prevention of colds;
- prevention of ear diseases;
- dental and speech therapy care.
Psychotherapy for parents
It is carried out for the child’s parents, who often blame themselves for what happened. Doctors of the relevant specialty talk with parents, explaining that such a defect can be easily corrected with surgery. If necessary, they resort to various psychotherapeutic techniques.
Organization of feeding
It is very important to keep food and drink out of your nose. To do this, take measures appropriate to the degree of the defect. So, for small defects, either special breast shields can be used, or special nipples that are put on a bottle (it is still advisable to feed the baby with expressed mother’s milk, which contains many times more nutrients than formula) and will cover the cleft palate.
In case of large defects, a probe is used - a tube that is inserted into the nose and which will reach the stomach. Such a probe is installed only in a hospital, they teach how to use it. The probe should be repositioned every 3 weeks to reduce the risk of complications associated with it. As soon as possible, such children need to have an obturator installed - a plate that will cover the defect.
Prevention of colds and ENT diseases
Until surgery is possible, a child with a cleft palate:
- must visit an ENT doctor every month if there are no complaints. If you have discharge from the nose, ears, or increased body temperature, immediately contact the same doctor;
- should not go to the garden at the slightest sign of ARVI;
- undergo hardening procedures;
- come to routine examinations, especially in the cold season, wearing a mask;
- Keep your baby's nose clean so that there are no food residues left there.
In some cases, an ENT doctor may recommend the installation of a special tube that will prevent middle ear infections.
Dental care
Children with a cleft palate should start brushing their teeth as soon as they appear, using a special silicone finger brush. You need to visit a dentist every year and, if necessary, carry out orthodontic correction using plates, braces or other devices recommended by an orthodontist.
Classes with a speech therapist
From the age of two, children with cleft palate need periodic speech therapy sessions to learn how to pronounce sounds and breathe correctly. On the recommendation of a speech therapist, parents work with the child at home.
Operation
The type of intervention is determined by the type of defect. Typically, 2 types of surgery are used for cleft palate: veloplasty (stitching of the soft palate) and uranoplasty (removal of the defect of the hard palate).
Veloplasty
It is recommended to perform it from 8 months of a child’s life (can be done from 1 to 2 years), while he is not yet trying to speak properly: performing the operation later can lead to the appearance of speech defects. It allows the child to restore swallowing and breathing.
The operation consists of suturing the defect of the soft palate with previously prepared triangular tissues taken from the oral mucosa.
This intervention is considered not very traumatic, so after 2-3 days you can introduce nutrition in the usual way instead of tube feeding. When this is successful, the probe is removed and the child is discharged.
Uranoplasty
The purpose of this operation is to lengthen the soft palate and narrow the middle part of the pharynx. If the defect is large, the intervention is carried out in several stages. The first stage can be carried out at 6 months. Additional interventions are carried out from 2 to 4 years.
For non-through clefts, the first stage is performed at 3-5 years. For through-and-through unilateral defects, intervention is performed at 5-6 years. If the defect is bilateral, 2 stages are usually needed, six months apart.
It is optimal to carry out interventions before 6 years of age, before the child starts school. After 6 years, cosmetic surgeries and cosmetic manipulations (for example, laser scar removal) can be performed. It happens that complete elimination of a cleft palate is completed only by the age of 18.
Uranoplasty consists of the following stages:
- incisions on both sides of the cleft with detachment of the mucous membrane;
- a Z-shaped incision is made, with its help the incisions are connected - the defect is closed;
- cutting off the nasal mucosa from the hard palate and moving it back;
- separation of muscle tissue from the sides of the pharynx and its movement to the middle;
- suturing the nasal mucosa, then suturing the muscles and nasal mucosa;
- suturing areas of the hard palate;
- treating the palate with an antiseptic;
- placing a plate on the palate to protect against infection. The plate is attached with a bandage, which is fixed on the head of the person being operated on.
Contraindications and complications
Cleft palate in children, photos of which show the structural features of the palate, can be treated surgically at an early age.
But there are contraindications to the operation:
- congenital heart defects - until they are corrected;
- other severe congenital malformations of internal organs;
- anemia;
- pneumonia.
If these contraindications are corrected or completely eliminated, the operation is possible. But for this you need to take additional tests to check the child’s condition.
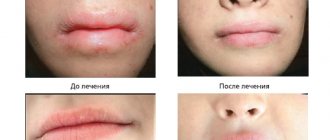
Cleft palate in children can be successfully treated. In the before and after photos you can see the result of the corrective work carried out on time. But there are cases when postoperative complications arise. Most often they arise due to medical error.
Complications include:
- divergence of seams at the junction of tissues. In this case, a repeat operation is performed;
- parts of tissue taken from other parts of the body may not take root and die. This problem can also be solved by repeated surgery;
- the appearance of rough scars, the severity of which is regulated by cosmetic procedures;
- Shortening the soft palate affects speech development. Therefore, in the postoperative period, the child attends speech therapy classes.
But complications after operations do not always occur and they can be eliminated so that the rehabilitation period is successful. To minimize the occurrence of complications, anamnestic data is collected.
The prognosis after the operation is favorable. After uranoplasty and veloplasty, it is possible to completely correct the cleft palate. If all recommendations are followed during the rehabilitation period, the baby’s development will be no different from his peers. But the child will be able to completely stop visiting doctors only by the time the bones finish forming.
A pathology such as cleft palate in children is very rare and can be successfully treated. Photos before and after the operation confirm the success of the treatment, provided that all medical recommendations are followed. It must be comprehensive so that the child grows up physically and mentally healthy.
After operation
After the operation stage is completed, the child remains in the hospital for some time (on average, about 3 weeks). For the first 2-3 days you need to remain in bed, and for about 10 days you must remain silent. Painkillers and antibiotics are also administered, bandages are carried out every 2-3 days, care is taken to ensure that there is no accumulation of mucus, saliva and blood in the palate (so that it does not suppurate later).
From the 5th day, massage of the suture is prescribed with a treated antiseptic: the index finger of the parent or the child himself is stroked and rubbed, then zigzag movements are performed along the mucous membranes in the place where the hard palate connects with the soft palate. It will also be necessary to perform some exercises aimed at providing anatomical conditions for speech development. This kind of gymnastics is painful to perform, so parents should ensure that it is performed correctly and regularly.
After being discharged home, parents need to go to the clinic, where rehabilitation measures will be prescribed:
- classes with a speech therapist, including improving articulation, developing the soft palate, learning to breathe through the nose;
- performing special exercises;
- speech therapy massage;
- physiotherapy;
- feeding using an orthodontic pacifier with a cut.
It is possible to assess what the cleft palate will look like before and after surgery only after 3-4 weeks, when the swelling from the reconstructed tissues has subsided. The scar on the face will decrease within another 2-3 months, and subsequently it can be corrected with laser.
Surgeries to correct cleft lip and palate in children
The main basic operations for the correction of congenital cleft lip are cheiloplasty and cheilorhinoplasty.* They differ in the volume and methods of surgical interventions performed, and are performed according to strict principles, but with individual characteristics.
To eliminate the cleft of the upper lip, reconstructive cheilorhinoplasty is mainly performed, which allows restoring the anatomical integrity of the organ while ensuring the functional component and creating optimal prerequisites for aesthetic well-being.
All surgical interventions are included in the basic compulsory medical insurance program and are absolutely free for parents of children from all regions of the Russian Federation.
- 1. Cheiloplasty.
An operation used for partial cleft lip without significant deformation of the nasal vestibule and its cutaneous-cartilaginous section. - 2. Rhinocheiloplasty.
The operation, used for complete cleft lips and in the presence of severe deformation of the nasal vestibule and its cutaneous-cartilaginous part, can be combined with periostoplasty for cleft lip, alveolar process and palate. - 3. Uranoplasty.
An operation used for partial and complete cleft palate, in which the hard palate and soft tissues of the velum are restored.
All operations are performed using multicomponent combined intubation anesthesia and last on average from 1.5 to 3 hours. The child's stay in the hospital is usually 8 - 10 days. Within 3–5 days after the operation, the swelling of the soft tissues subsides, the child’s condition improves, and he gradually adapts to new living conditions.