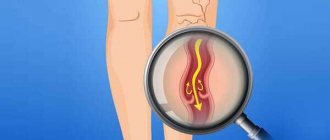
A single lesion in the lungs (SLP) is defined as a local area of compaction of lung tissue of a round or similar shape with a diameter of up to 3 cm [15]. This international definition differs from the traditional domestic concept of pulmonary lesions, the source of which is phthisiatric practice (in the classification of pulmonary tuberculosis, the size of lesions does not exceed 1 cm, and larger lesions are defined as infiltrates, tuberculomas and other types of changes) [14, 15].
Pathological formations of the lungs of small size (up to 2 cm) in most cases are detected during computed tomography of the chest, performed for various reasons [10, 11, 14, 16-18].
Some characteristics of space-occupying lesions on CT allow us to judge their nature - benign or malignant, but they are not decisive when making a diagnosis [19]. The nature of the formation can also be judged by the rate of its growth [20].
Meanwhile, based on the results of one CT study, it is often difficult to make a differential diagnosis; repeated studies over time are required. During the inflammatory process, the lesions disappear after 1-2 months. In the case of atypical glandular hyperplasia, the lesions do not change for several years. In adenocarcinoma, increased size and/or increased density as well as vascular convergence may be seen [11, 12].
Focal formations in the lung tissue discovered during such an examination often remain unattended by specialists, which sometimes leads to disappointing results of treatment for this category of patients.
The difficulties of accurately diagnosing focal lung formations are well known - differential diagnosis most often has to be made between peripheral cancer, benign tumor (hamartochondroma, etc.), tuberculoma, sarcoidosis, and metastatic lesions of the lung [1-4, 6, 7, 10, 12].
According to S.V. Miller et al. [8], diagnostic thoracotomy is the final method of comprehensive examination of patients with small round lung formations and provides truly early diagnosis and timely surgical treatment. Consequently, radical surgical intervention undertaken for a round formation in the lung, the genesis of which is unclear, is a method that allows for morphological verification of the early stage of a malignant tumor and performing organ-preserving surgery.
Other authors believe that currently there is no unified approach to determining the nature of focal lung formations. Obviously, with a high risk of a malignant tumor, the optimal approach is the earliest possible morphological verification of the diagnosis. In case of low risk of malignant process, it is more rational to carry out dynamic observation [11].
The result of these actions may be the identification of a group of patients with an obviously benign process, as evidenced by the absence of growth dynamics of the lesion for 2 or more years, the presence of “benign” calcifications, inclusions of fat (hamartoma) or fluid (cyst) in the lesion according to CT data. In such a situation, only observation is necessary. This also includes cases of arteriovenous malformations and other vascular changes, as well as inflammatory processes in the lungs (round tuberculous infiltrate, tuberculoma, mycetoma, etc.), requiring specific treatment [5, 9, 13].
The second possible result is the detection of signs of a malignant process (a lesion with a diameter of more than 1 cm with radiant uneven contours, lesions of the ground glass type and mixed solid type, which should be regarded as potentially malignant), for which morphological verification is necessary in a specialized medical institution [12] .
Every year in Russia over 63 thousand people, including over 53 thousand men, become ill with lung cancer. In more than 20 thousand patients (34.2%), lung cancer is detected at stage IV, so the task of detecting malignant lung tumors in the early stages of their development is extremely relevant [2, 7, 8].
A threatening factor when diagnosing small-diameter lung tumors is their asymptomatic nature. The absence of complaints, the meager clinical picture of the disease, difficulties with prevention and primary detection of lesions make the problem of lung formations up to 2 cm in diameter relevant for scientific research and practically significant for preserving the health and often the lives of patients.
General information
Hamartoma is a benign neoplasm that can affect any organ.
The disease is extremely rare in females; hamartoma is most often diagnosed in men aged 20-40 years and in children. Structurally, the neoplasm consists of organ tissue and may contain blood vessels, fibrous formations, cartilage or adipose tissue. The hamartoma has a round shape, the surface can be smooth or bumpy.
A lumpy benign neoplasm is formed in the organ during embryogenesis. Most often, the pathological process is detected in the pulmonary system, hypothalamus, and mammary gland. It is extremely rare that hamartoma is diagnosed in the liver and spleen.
Pathological anatomy
Macroscopically, the hamartoma is most often round in shape, its surface is finely lumpy or smooth, and the consistency is dense-elastic or dense. There is no capsule. Clear demarcation from adjacent lung tissue. On the section, the tumor has a grayish or gray-yellow tint, and has a lobular appearance. The tumor includes foci of cartilage and is separated by fibrous layers; lime inclusions are often found (according to the book “Thoracic Surgery: A Guide for Doctors,” edited by L.N. Bisenkov).
In some cases, a hamartoma removed from its bed breaks up into separate lobules. The compressed alveoli form the tumor bed. There is no anatomical connection between them and the tumor, which explains the possibility of enucleating the hamartoma during surgery.
Microscopically, hyaline, and in rare cases, elastic cartilage, which has an atypical structure, is determined; there are layers of connective and adipose tissue around it. Areas of calcification or ossification are also detected. Sometimes there are lymphoid accumulations, smooth muscle fibers, and cyst-like cavities lined with epithelium.
Pathogenesis
A hamartoma is formed as a result of a violation of cell development in the embryonic period and consists of various elements of embryonic tissues. The development of a tumor is associated with a violation of organ formation and tumor-like growth of tissue components around the future organ.
Despite the early formation of tumor sprouts in the embryonic period, hamartoma may not manifest itself until the patients reach adulthood. The neoplasm consists of the same elements as the organ itself, but is characterized by an incorrect arrangement of components and an unhealthy degree of differentiation. This is what distinguishes a hamartoma from a teratoma , which contains tissue buds that are foreign to a given organ.
Likely consequences
Despite its benign nature, the lack of timely removal is dangerous due to malignant transformation, the development of obstructive pneumonia, segmental or lobar atelectasis. In rare cases, the hamartoma rapidly increases in size, causing metastases to occur in the liver, spine and diaphragm.
If the pathology is started, the hamartochondroma degenerates into chondrosarcoma, liposarcoma, adenocarcinoma or fibrosarcoma. These malignant tumors are deadly for the patient.
Classification
The generally accepted classification is based on the predominance of certain tissues in the neoplasm.
Types of hamartomas indicating the predominant tissue:
- lipomatous (fatty);
- chondromatous (cartilaginous);
- fibromatous (connective);
- leulomyomatous (smooth muscle);
- organoid (several types);
- angiomatous (vessels).
Depending on the number of pathological formations, single and multiple foci are distinguished.
Lung hamartoma
Congenital, benign neoplasm. The tumor can contain both lung tissue and adipose, cartilage tissue, as well as blood vessels and fibrous formations. It is considered the most common species among hamartomas.
The pathological process is formed against the background of mutation at the level of growth and differentiation of tissues during gestation in the fetus. After birth, the pathological node continues to grow and develop. The first symptoms may only appear decades later. It is easiest to diagnose a node that contains cartilage tissue. The neoplasm can also include alveolar, epithelial, connective and other types of tissue. The parenchyma is affected subpleurally (on the surface) or intrapulmonary (in the deep layers). Most often, the node is located in the lower lobe of the right lung.
The formation is considered absolutely benign; metastases are not diagnosed. Lung tissue can be damaged only when the tumor a large size. Typically, nodes do not exceed 40 mm in diameter, but in medical practice large neoplasms up to 100 mm are also encountered.
Hypothalamic hamartoma
The hypothalamus is located between the floor of the third ventricle and the diencephalon. This area of the brain is responsible for the functioning of the internal glands and other vital systems. Any structural changes in the hypothalamus lead to serious disruptions in the functioning of the entire organism.
A hypothalamic hamartoma is a benign compaction that consists entirely of organ pathogens and does not contain foreign inclusions. As the hamartoma increases in size, adjacent tissues are compressed, which can negatively affect the patient’s health.
A neoplasm in the hypothalamus also originates at the embryonic stage. The first signs of pathology may appear already in the first year of a child’s life. The cause of the development of hypothalamic hamartoma is considered to be the negative impact of external factors on the body of a pregnant woman, which leads to cell mutation in the fetus.
Hamartoma of the breast
The formation of the neoplasm also begins during the development of the embryo. Breast hamartoma is considered a benign tumor, but it can bring some discomfort to a woman’s life. A cystic neoplasm consists entirely of tissue from the own mammary gland. The first symptoms appear after 30 years. The pathological node is easily palpable, has clear boundaries and moves freely (if its size is more than 30 mm). May cause pain when palpated. Ultrasound examination reveals it as a dense, lumpy formation.
Liver hamartoma
The formation of a benign tumor occurs during the formation of the embryo. At the initial stage, the disease is completely asymptomatic. In 7% of patients, malignancy occurs and the tumor turns cancerous. The disease is detected in childhood. The tumor looks like a dense, lumpy formation. Depending on the structural composition, two varieties are distinguished:
- mesenchymal;
- hepatocellular.
Classification of liver hamartoma by location in the organ:
- near-surface;
- deep;
- subcapsular.
It is also customary to distinguish cystic and fibrous hamartomas, true and biliary tumors.
The danger of the disease lies in the risk of rupture of the neoplasm and the very rapid proliferation of pathological cells. Compression of neighboring organs and tissues is possible. It is important to pay attention to signs such as:
- attacks of nausea;
- excessive thinness;
- fast fatiguability;
- stool instability (alternation of constipation , diarrhea and vice versa);
- muscle weakness.
Hamartoma of other organs
The neoplasm can be located in other human organs and tissues:
- spleen;
- retina and iris (astrocytic form);
- nose (nasal form);
- esophagus, stomach, large intestine (presacral form);
- sebaceous glands;
- The lymph nodes;
- skin of the thighs, buttocks, arms, legs, face (cutaneous hamartoma);
- renal system ( angiomyolipoma ).
1.General information
Medical terms ending in “-oma” (lipoma, melanoma, fibromyoma, and many others) mean a tumor or, more precisely, neoplasia - a neoplasm not intended by nature in any organ or tissue. As is known, such structures can be malignant or benign; The distinctive characteristics of the latter are that they retain a certain cellular similarity to the tissue from which they develop (at the same time, they grow much slower than cancerous tumors), do not show a tendency to grow into adjacent structures and do not metastasize, i.e. do not create new foci from their cells that spread through the blood or lymph flow.
A hamartoma, or cartilaginous tumor, is a benign formation that forms in the lung during fetal development. The first detailed clinical descriptions of this congenital anomaly date back to the beginning of the 19th century, but all of them were made based on the results of post-mortem studies. Intravital diagnosis of hamartoma became possible only a century later, with the advent of the first of the imaging diagnostic methods, i.e. fluoroscopy and radiography.
In addition to parenchymal lung cells, hamartoma may contain cartilaginous, connective, and fatty components. Accordingly, its various types are classified (lipomatous, fibromatous, etc.). The shape is usually round, the dimensions vary from five to fifty or more millimeters. An upward trend is considered rare; according to other sources, very slow growth, on the contrary, is typical for hamartomas. Cases of malignancy (malignancy) are sporadic, isolated phenomena.
Hamartomas make up about 10% of the total volume of all registered pulmonary neoplasms and are the most common benign lung tumor.
A must read! Help with treatment and hospitalization!
Causes of hamartoma
The mechanism of development of the neoplasm is associated with a violation of the formation of organs during intrauterine development. Pathology can develop under the influence of unfavorable life factors, due to mutations , or against the background of a hereditary predisposition.
During embryonic development, the process of growth and division of cells in the organ is disrupted, which leads to their spontaneous proliferation and improper differentiation. The growth of the neoplasm begins from the moment the child is born and may not manifest itself in any way for several decades.
Causes of pulmonary hamartoma
Pulmonary hamartoma develops against the background of a malformation of the pulmonary system associated with a violation of the formation and formation of bronchopulmonary structures during embryogenesis. The cartilaginous, connective tissue and smooth muscle components of the lung hamartoma take their development from the mesenchyme - the embryonic tissue. Secondarily, epithelial structures are involved in the pathological process during the growth of the tumor.
Predisposing factors are also considered to be gene mutations, genetic predisposition, prolonged exposure to negative factors (ionizing radiation, hazardous chemicals, etc.).
Fibrous hamartoma in children
The neoplasm occurs during intrauterine development. The exact causes of fibrous hamartoma are still not understood. However, many doctors associate the development of pathology with heredity, gene mutations and the impact of unfavorable facts on the embryo.
Symptoms of the disease:
- periodic cough;
- mild chest pain;
- dyspnea;
- hemoptysis (manifests itself as the disease progresses).
The tumor is usually discovered accidentally after an x-ray or examination for another disease. To clarify the diagnosis, the doctor may prescribe an ultrasound, MRI, electroencephalographic study and fibrobronchoscopy.
Treatment of fibrous hamartoma in children consists of constant medical supervision, symptomatic therapy (for exacerbation of symptoms) and surgery (for progression of the disease).
Symptoms of hamartoma
The peculiarity of hamartoma is that the pathological process does not manifest itself in any way for a very long time. The patient seeks medical help only when unpleasant symptoms significantly impair the quality of life. For example, when a tumor reaches a gigantic size and compresses the affected organ or adjacent tissues, which leads to disruptions in their functioning.
Symptoms of pulmonary hamartoma:
- severe shortness of breath ;
- discomfort and pain behind the sternum;
- cough with purulent or bloody discharge;
- pain during inhalation and exhalation.
Symptoms of hypothalamic hamartoma in childhood:
- poor learning ability, restlessness;
- disturbances of memory, thinking, attention and motor activity;
- epileptic seizures , convulsions ;
- loss of consciousness;
- feeling of anxiety and restlessness;
- emotional instability in the form of outbursts of aggression or depression ;
- early puberty;
- disturbances in the functioning of the endocrine system.
Symptoms of a hypothalamic tumor in women:
- gynecomastia;
- amenorrhea;
- galactorrhea;
- thyrotoxicosis;
- uterine bleeding.
Symptoms of liver hamartoma:
- indigestion;
- weight loss;
- constipation, diarrhea;
- periodic feeling of hunger;
- palpation of the tumor or its protrusion when the hamartoma reaches a large size.
Clinical symptoms are extremely mild.
Symptoms of mammary gland hamartoma:
- protrusion of the tumor from the side of the mammary gland when the tumor reaches a large size (cosmetic defect);
- mobility and painlessness of the tumor when palpated.
Hamartoma can manifest itself in completely different ways depending on the specifics and functionality of the affected organ. Neoplasms in the hypothalamus and pulmonary system accompany patients with specific symptoms for a long time.
Hamartomas of the hypothalamus and hepatic system manifest themselves already in childhood. Tumors in the mammary glands and liver manifest themselves very weakly clinically, and the patient is in the dark for a long time about the true cause of the unpleasant symptoms.
Diagnostics
To identify hamartochondroma, an X-ray examination, computed tomography, magnetic resonance imaging of the lungs and transthoracic puncture biopsy are performed, followed by histological examination of the biological material.
An X-ray with a tomogram can easily identify a single hamartoma of small size, round in shape, with clear boundaries and a peripheral location. The surface of the defect is smooth or hilly.
The disease is divided into several radiological variants - shadows of medium and high intensity with compaction in the center, homogeneous structure. With large defects, the pulmonary pattern is enhanced due to the convergence of the branches of the bronchi and blood vessels.
Endoscopic bronchoscopy is used only for endobronchial tumor localization. To confirm the benign nature of the hamartochondroma, a histological examination of a piece of the tumor obtained during thoracotomy, transthoracic puncture biopsy or thoracoscopy is performed.
The taken material contains immature cartilage tissue, epithelial cells, minor connective structures and fat droplets.
During dynamic observation over a long period of the tumor, an extremely slow increase in formation is detected or excluded.
It is important to distinguish the disease from various malignant lung tumors, cancer metastases of other organs, cystic lesions or true benign pathologies. In case of hamartochondroma, the patient should consult with a pulmonologist, oncologist, phthisiatrician and thoracic surgeon.
Tests and diagnostics
Any neoplasm causes some concern, especially if its true nature is unknown. Certain diagnostic research methods make it possible to determine the exact location and nature of the tumor.
When examining a patient, the doctor pays attention to factors such as:
- severity of reflexes;
- skin sensitivity;
- full functioning of the vestibular apparatus;
- muscle tone, balance, proper coordination of movements.
The patient must undergo tests to determine the level of sex hormones.
Instrumental methods for diagnosing hamartoma:
- radiography (for pathology of the pulmonary system);
- ultrasound examination (if tumors are suspected in the mammary glands, abdominal organs);
- fibrobronchoscopy (if pathology in the lungs is suspected);
- MRI or CT (diagnostic search in the hypothalamus).
Various research methods make it possible to determine the exact location of the tumor. Quite often, a diagnostic search is difficult due to the small size of the pathological focus, as well as the location of the abnormal node inside the organ (hypothalamus, lungs) and the similarity of the cellular composition of the tumor with healthy tissues of the organ.
Which method of diagnosing pulmonary hamartoma to choose: MRI, CT, X-ray
Selection Methods
- X-ray,
- CT.
What will a chest x-ray show for hamartoma?
- The solitary node is round in shape, of various sizes (usually <4 cm), with smooth or jagged, clearly defined boundaries, having a lobular structure, without reaction from the surrounding tissue
- Usually located on the periphery (in 90% of cases; very rarely - endobronchial)
- In approximately 15% of cases, pulmonary hamartomas contain foci of calcification that resemble “puffed corn” in shape.
What will CT scans of the chest show for hamartoma?
- Changes are the same as with radiography
- The high sensitivity of CT can detect calcification of the cartilage and fat contained in the hamartoma.
Features
- A nodule with smooth, clearly defined edges, containing foci of calcification that resemble “puffed corn” in shape, and does not cause a reaction from the surrounding tissue.
Treatment of hamartoma
Treatment tactics largely depend on the location of the tumor, its size and volume, as well as clinical symptoms.
If the tumor is small and the clinical picture is mild, regular medical observation is sufficient. However, most often treatment for hamartoma is aimed at removing the tumor.
Treatment of pulmonary hamartoma
- in case of peripheral localization of the tumor, curettage or partial resection of the affected organ is performed;
- when a pathological node is located near the root of the lung or in its depth, as well as when several nodes are identified at once, they resort to removing a lobe of the lung. In some cases, complete removal of the organ is necessary;
- in case of damage to the bronchi, surgical treatment is carried out using cryodestruction, electrocoagulation, and laser. The goal is to remove the pathological area while preserving as much of your own healthy tissue as possible.
Treatment of hypothalamic hamartoma
A neoplasm in the brain poses a particular danger, which requires timely and competent treatment. Therapy can be carried out medically or surgically depending on the diameter of the tumor.
Drug therapy can reduce the severity of negative symptoms and eliminate convulsive syndrome. Drug therapy is also used before surgery.
Modern medicine allows, through radiosurgical treatment, to avoid excessive brain trauma during tumor removal. Using a tomograph, the operating doctor monitors the direction of the radiation beam. This technique is very popular because... avoids craniotomy and preserves brain tissue as much as possible. Radiosurgical treatment is especially important in patients with a high risk of complications and those in difficult situations.
Treatment of hamartoma of other localization
When hamartoma affects other organs and tissues, surgical treatment is most often used. Surgical intervention is necessary primarily for differential diagnosis of the identified neoplasm (for example, with damage to the mammary glands).
Treatment
Since the diagnosis can finally be made only after a histological examination of the removed hamartoma, the main method of therapy is surgical, that is, surgery. Subpleurally located hamartomas are removed by simple enucleation with a previous incision of the pleura above them and the cortical layer of the lung. In recent years, this operation has been performed using video-thoracoscopic techniques, avoiding traumatic incisions.
When the hamartoma is located endobrochially, in some cases they resort to excision of the tumor during fiberoptic bronchoscopy. If there are significant contraindications to the operation, the doctor can only prescribe long-term follow-up.
Prevention
Due to the fact that the tumor-like node begins to form during embryonic development and is partly due to genetic factors, there is no specific prevention.
It is almost impossible to predict in advance at what stage of development a failure will occur. However, parents can make their contribution to the birth of a healthy baby. To do this, it is necessary to minimize all risks associated with the negative impact of the environment on the health of the expectant mother.
Parents are advised to adhere to a healthy lifestyle, give up bad habits, and unquestioningly follow the instructions of the attending physician. Particular care should be taken when taking medications, especially during pregnancy.
Only with the right organizational approach to bearing and giving birth to a baby can the risk of developing pathology be significantly reduced, even with a genetic predisposition to neoplasms.
results
85 lobectomies, 10 segmentectomies, 3 hamartochondroma enucleations and 1 marginal resection were performed. The distribution of operations by nosological groups is contained in Table 4.
Table 4. Structure of completed operations
Features of performing robot-assisted operations for pulmonary tuberculosis
One of the main conditions for performing operations for pulmonary tuberculosis was the presence of an adequate preoperative course of anti-tuberculosis chemotherapy, taking into account the data of the National Clinical Guidelines 2.
At the stage of mastering the surgical technique, among the first interventions was marginal lung resection, performed according to relative (social) indications for the subpleural location of tuberculoma in the upper lobe of the right lung. At the same time, further use of robot-assisted four-port access with minimal changes in the lungs was considered inappropriate, given the lack of advantages over routine VTS.
Robot-assisted segmentectomies for tuberculosis were also performed during the learning curve. The operating time for segmentectomies ranged from 65 to 320 minutes, intraoperative blood loss ranged from 10 to 200 ml. Out of 8 operations, access conversion was performed in 2 cases: during resection of 1-2 segments of the right lung due to bleeding (volume - 1200 ml) caused by double failure of the intersegmental border with a stapler, and during resection of 1-2 segments of the left lung for suturing a bronchonodular fistula of the culminating bronchus, formed during the removal of an enlarged lymph node. In this group of patients, one surgical complication was observed—delayed expansion of the operated left lung, which required drainage of the pleural cavity.
The most common procedure for tuberculosis was robot-assisted lobectomy. The total intervention time ranged from 85 to 380 minutes, intraoperative blood loss ranged from 20 to 500 ml. The rate of major surgical complications was 13.3% (10 patients). The structure of complications was dominated by prolonged release of air through drains and atelectasis, which required sanitary fibrobronchoscopy.
The main features of anatomical lung resections for tuberculosis are fibrous changes in the elements of the lung root, the presence of adhesions in the pleural cavity and calcified bronchopulmonary lymph nodes.
In the study group, 67 of 84 (79.8%) patients had pleuropulmonary adhesions, and 5 of them (7.5%) had total fusion of the pleural cavity. In 10 patients, it was necessary to isolate the lung in the extrapleural layer in a limited area (usually at the apex of the pleural cavity). However, only in one case was conversion to lateral thoracotomy performed - in the presence of a parietal mooring more than 1 cm thick, when it was impossible to create a free space sufficient for the robot to operate.
In most interventions using robot-assisted access, it was possible to safely treat elements of the lung root, despite peribronchial and perivascular fibrosis in the lung root. During lobectomies, 2 patients had a need for access conversion. In the first case, this was a patient with a hilar location of the cavity and lymphadenopathy of the hilar lymph nodes, when it was impossible to find a safe layer for dissection of the arteries of the upper lobe of the left lung. The second patient required emergency access conversion due to damage to the anterior wall of the pulmonary artery on the left during dissection of the upper lobe bronchus.
For unilateral pulmonary tuberculosis, robot-assisted resection was the main step. After this, the patient resumed anti-tuberculosis chemotherapy with correction in accordance with the data on the drug sensitivity of MBT obtained from the surgical material.
For bilateral tuberculosis, robot-assisted pulmonary resection was performed as one of the stages of surgical treatment: in one patient in combination with valvular bronchoblocking on the opposite side; in five - in combination with minimally invasive anatomical resections of the contralateral lung. No access conversions were required in this group. Postoperative complications were reported in half of the patients and included prolonged air release (2 cases) and uvular segment vein thrombosis after resection of C1–3 of the left lung (which required reoperation using a video-assisted thoracoscopic approach using a left upper lobectomy type).
All patients were discharged to continue treatment in a therapeutic hospital/sanatorium in satisfactory condition without signs of active tuberculosis inflammation.
Features of robot-assisted lung resections for congenital lung malformations
At the stage of mastering the robot-assisted access technique in 2013, the first operations were performed, including for therapeutic and diagnostic purposes, on patients with peripheral tumors. At the same time, precision removal of hamartochondromas was performed in 3 patients (Fig. 2).
Rice. 2. Endophotogram of an enucleated hamartochondroma. Photos of the authors
The operation time ranged from 175 to 230 minutes with no significant blood loss (less than 10 ml). One access conversion was performed when it was impossible to identify the area of pathological changes during instrumental palpation. Subsequently, robot-assisted access was not used for this pathology due to the lack of significant advantages over routine VTS.
One operation was performed for cystic hypoplasia of the upper lobe of the left lung (duration - 155 minutes, blood loss - 10 ml). A distinctive feature was a pronounced adhesive process in the upper parts of the left pleural cavity. At the same time, the advantages of robot-assisted access made it possible to perform precision pneumolysis in the extrapleural layer without opening lung cysts.
Three patients were operated on for intralobar sequestration of the lung. In 2 cases there was a secondary infection with non-tuberculous mycobacterium, which required a preoperative course of antibiotic therapy. In 2 cases, lower lobectomy was performed on the left, and in one case, lower lobectomy was performed on the right. The number of aberrant vessels coming from the abdominal aorta ranged from 1 to 3 (Fig. 3).
Rice. 3. Preoperative spiral computed tomography of the chest organs. Photos of the authors. A, B - axial projection. C - frontal projection. D — sagittal projection. Note. The arrow indicates the sequester and aberrant vessel
The total operation time was 130–515 minutes. The main features were precision dissection of the inferior pulmonary ligament and suturing/clipping of the aberrant vessel (Fig. 4).
Rice. 4. Stages of robot-assisted lobectomy for intralobar sequestration. Photos of the authors. A, B, C - isolation and processing of aberrant vessels. D — isolation of the inferior pulmonary vein. E - highlighting the artery of the lower lobe. F - isolation of the lower lobe bronchus
There were no postoperative complications requiring additional interventions. In one case, there was a prolonged release of air through drains (more than 5 days), which stopped on its own. Based on the results of a bacteriological study of the drug, the course of antibiotic therapy was adjusted in patients with a combination of congenital lung malformation and mycobacterial infection. A photo of the preparation is shown in Figure 5.
Rice. 5. Operative preparation. Photos of the authors. A, B - sectional view. C—general rear view of the specimen. D — general view of the preparation from the front. Note. The arrow indicates the sequester
Features of robot-assisted lung resections for chronic nonspecific lung diseases
For localized bronchiectasis and chronic abscesses, 6 lobectomies and 2 segmentectomies were performed. The duration of the operation ranged from 95 to 380 minutes, surgical blood loss was 10–220 ml. In all cases, an adhesive process was detected. In addition, the main feature of the operation for these pathologies was the need for careful treatment of hypertrophied bronchial arteries (Fig. 6).
Rice. 6. Stage of treatment of the bronchial artery during right lower lobectomy for bronchiectasis. Photos of the authors. A - isolation of the bronchial artery. B — clipping of the bronchial artery. Note. RLLB - bronchus of the lower lobe of the right lung; the arrow indicates the hypertrophied bronchial artery
The only conversion was performed according to emergency indications due to a traction tear of the anterior wall of the left pulmonary artery in a patient with bronchiectasis in the intimate location of enlarged lymph nodes (previously, the patient had undergone a course of radiation therapy to the breast area due to a malignant neoplasm, as well as multiple courses nonspecific antibiotic therapy for exacerbation of nonspecific infection). A surgical complication was also recorded in one patient - prolonged release of air through the drains, which required re-drainage of the pleural cavity.
Consequences and complications
Hamartoma is characterized by gradual growth. The tumor is characterized by extremely slow growth, so patients do not show any complaints for a long time. Complications can occur if the tumor grows excessively. Increasing in size, the hamartoma disrupts the functioning of not only the organ in which it is located, but also in nearby organs and tissues due to compression.
When a hamartoma is located in the lungs, damage can be caused to the bronchial tree, the lumen of which is compressed under the influence of growing tumor tissue. When identifying multiple nodes, the doctor faces a very important task - to exclude a rare genetic pathology - Cowden's disease , which is characterized by the formation of tumors in other internal organs and tissues.
The danger lies in the risk of malignancy, which is accompanied by the appearance of papillomas and warts on the mucous membranes and skin.
If a hypothalamic hamartoma is located in the diencephalon, then the patient may experience mental disorders, loss of consciousness, inappropriate behavior, and convulsive activity.
If the hamartoma is located in the liver, then internal bleeding may occur when the tumor grows and ruptures. With the accelerated growth of a liver hamartoma and the filling of its contents with cystic components, there is a high risk of developing cancer.
In case of breast hamartoma, it is also extremely important to carry out timely differential diagnosis to exclude breast cancer .
Instrumental diagnostics
An x-ray is required. A hamartoma is visible as a single (or multiple) spherical shadow (of solitary pulmonary nodes), having clear, slightly wavy contours. With a lobular structure, the tumor has a tuberous outline. Typical are calcareous inclusions, which are localized as individual grains or a central conglomerate.
The shadow in the center of the tumor is often more intense than the shadow of the edges, which suggests that it is a hamartoma and not another tumor. The pulmonary pattern around the formation is often unchanged. Sometimes a rim may be detected along the periphery (tumor bed). There are no changes in the root of the lung, and there are also no pleural reactions. Whatever part of the lung tissue the hamartoma is localized in, its long axis in all cases is directed towards the root of the lung. If we carry out long-term dynamic observation, it can be noted that the size of the hamartoma changes very slowly, but the intensity of calcareous deposits often progresses.
Endobronchial hamartomas manifest themselves with direct and indirect signs. Straight is a spherical tumor-like formation in the lumen of the bronchus with smooth and clear contours, detected on X-ray tomography. Indirect manifestations are hypoventilation, atelectasis and other signs that indicate impaired bronchial obstruction.
Fiberoptic bronchoscopy
Endobronchial hamartoma can be localized in the area of the bronchial “spur” or on the walls of the bronchi. The shape is cone-shaped and gar-shaped, the color is whitish, the base is wide. The mucous membrane covering the hamartoma is unchanged. Instrumental palpation reveals a rocky density, which makes it difficult to take biopsy material from the tumor.
Forecast
The prognosis is considered favorable if the tumor is detected early and adequate therapy is received. In this case, the tumor does not increase in size, and the unpleasant symptoms are controlled with medication.
Hamartoma is a benign tumor that rarely undergoes changes at the cellular level and forms metastases. In world practice, there are about 20 cases of degeneration of a hamartoma into a malignant tumor - hamartoblastoma .
Chondromatous hamartoma of the lung
Lung hamartoma is a congenital benign tumor consisting of lung tissue, vascular structures and cartilage. There are three types of disease: endobronchial hamartoma, anterior peripheral and posterior peripheral.
In most cases, the symptoms are mild. Typically, the diagnosis is made by MRI or X-ray results. Sometimes the patient may complain of cough, slight shortness of breath and pain in the chest area. The diagnosis is made taking into account the medical history, general condition and the results of instrumental studies. Additional examination methods include puncture, which allows you to determine the status of the tumor, and biopsy. In contrast to biliary hamartoma of the liver, the diagnosis of chondromatous hamartoma of the lung is made three times more often.
Classification of the disease
Clinicians know several classifications of hamartoma. For example, division by predominant tissue suggests the existence of the following tumor types:
- cartilaginous or chondromatous hamartoma is the most common type (diagnosed in 50% of cases);
- fatty or lipomatous;
- bronchial, smooth muscle or leiomyomatous;
- muscular or fibromatous;
- vascular or angiomatous;
- mixed or organoid.
According to the number of hamartomas there are:
- single;
- multiple - are extremely rare.
Depending on the location of appearance, it happens:
- peripheral or parenchymal hamartoma - most often localized in the area of the right lobe of the lung;
- endobronchial hamartoma or located in the walls of the bronchi - occurs in isolated cases, localized in the small bronchi;
- intrapulmonary hamartoma - can form in the hilar, middle or cortical zone of the lung;
- subpleural hamartoma - located on the surface, often in the area of the apex of the lung.
Based on the severity of clinical signs, clinicians distinguish several degrees of severity:
- mild - asymptomatic;
- moderate - symptoms are scanty, less often completely absent;
- severe - characterized by pronounced symptoms, which is due to the growth of the tumor and compression of surrounding tissues.
Pathogenesis of the disease
A hamartoma in the lung forms in the 4th - 6th week of fetal development. Due to reasons that have not been fully identified, the rudiments of smooth muscle, cartilage, vascular and other structures are involved in the structure of the respiratory organs. That is, components that are unusual for the respiratory organs are added, which belong to completely different organs.
Growth is usually extremely slow. Small nodules increase with the development of the respiratory system. Cases of sharp jumps in increased abnormal cell division have been recorded during hormonal disruptions, including during adolescence.
Treatment of the pathological condition
There is no medical treatment for pulmonary consolidation. Physiotherapy procedures are also ineffective; they can catalyze unwanted tumor growth. For the same reason, it is prohibited to use traditional medicine recipes.
It is important to maintain the condition (hormonal levels) with which the patient came to the pulmonologist. Otherwise, uncontrolled development of compaction will be provoked.
If a hamartoma interferes with the function of the respiratory system, and even more so develops into an oncological disease, doctors decide to surgically remove it.
The operation is performed using an endoscope, a minimally invasive radical method if the tumor is small. If it has reached an impressive size, surgeons perform a thoracotomy type of operation (an open incision is made in the chest).
Doctors excise the tumor and remove it completely. If organs are damaged, for example, blood flow is disrupted due to compression, a decision is made on partial or local resection of the lung lobes.
If the formation does not interfere and does not pose a threat, pulmonologists and surgeons take a wait-and-see approach. Surgical intervention on the respiratory system without reason is undesirable. If the patient has decided to remove the defect, resection is performed.
What is important to know about hamartoma?
Only 7% of the population, which is not related to medicine, knows what pulmonary hamartoma is. The pathology is included in ICD-10 and belongs to code D14.3 (Benign neoplasms of the bronchi and lung).
This is a round formation that clearly stands out against the background of the lung tissue. In appearance it resembles a smooth, sometimes lumpy, white-gray elevation. In cross-section, it resembles a capsule with viscous translucent contents, pronounced layers and yellowish spots. The consistency is dense.
Such capsules consist not only of lung tissue. Smooth muscle, adipose, vascular, connective and cartilage are involved. In 5% of cases, during a biopsy, specialists find bone tissue. Usually one of the components prevails over the others.
A hamartoma forms on the surface of the lung tissue or in its thickness. Development sometimes occurs suppleurally, that is, under the membrane of the pleura. The area underneath has been replaced with connective tissue due to various pathologies and injuries of the respiratory organ.
The size of the tumor rarely reaches 12 cm, most often the nodules are no more than 3 cm in diameter. Hamartoma is a solitary (single) formation, but there have also been situations where up to 15 small foci of abnormal development were found in patients.
The neoplasm is characterized by chaotic development. It practically does not melange into other organs and only in 3% goes into the malignant stage.
When asked what a pulmonary hamartoma is, back in the 1980s, pulmonologists answered that it was a deadly disease. However, research has experimentally proven that a tumor rarely leads to a decrease in the patient’s standard of living.
Causes of the disease
Among all benign neoplasms of this localization, pulmonary hamartoma occurs on average in 60% of cases. In most situations, the disease is diagnosed in people aged 30 to 50 years. It is worth noting that men are affected by the disease several times more often than women.
Currently, the mechanisms and causes of pulmonary hamartoma remain unknown. Many specialists in the field of pulmonology believe that such a tumor is a developmental defect that occurs against the background of a violation of the formation of internal organs at the stage of embryogenesis.
Main risk factors:
- burdened heredity;
- unexplained gene mutations;
- long-term influence on the parents’ body of mutagens, which include chemical and toxic substances, and ionizing radiation;
- severe poisoning and intoxication;
- uncontrolled use by future parents of medications that have a teratogenic effect.
The reasons behind the increase in tumor size throughout a person’s life have not been established.
Despite the fact that the formation includes cartilaginous and vascular, fatty and fibrous structures, its components are identical to those of a healthy lung. The differences are a different degree of differentiation and incorrect location.
A similar neoplasm of the left or right lung has the following characteristics:
- resembles a node surrounded by a capsule (less often without it);
- clear limitation from healthy tissues;
- shade - gray or yellowish;
- densely elastic consistency;
- lobular structure with fibrous layers;
- volumes can vary from 1 to 12 centimeters, but often the sizes are 5 centimeters;
- the composition may include glandular tissue, lymphatic cells and vessels, bone inclusions, and the presence of calcareous and cyst-like particles is possible.
The factors of malignancy of pulmonary hamartoma are not known to clinicians, but it is noted that degeneration develops extremely rarely - the chance of developing an oncological process is very low.
Symptoms
Signs of a hamartoma are noticed when it has already reached an impressive size. Symptoms appear if the tumor appears on the inner wall of the bronchus.
The clinical picture of the tumor is as follows:
- shortness of breath appears, first during physical exertion, and then at rest;
- feeling of a foreign object when inhaling;
- dry cough or attempts to cough;
- pain at the site of formation.
As the compaction grows, partial or complete disruption of respiratory function is observed. The cough is wet, the sputum is viscous and yellowish. In case of complications, hemoptysis and purulent discharge are added.
Pathology prognosis
The tumor rarely recurs; only 7% of cases of recurrent development of compaction after surgery have been recorded. Immediately after removal of the seal, regular examination by a pulmonologist is recommended for 2-5 years. Hamartoma is sometimes hidden, when even after diagnostic studies it is not immediately visible.
Painful symptoms disappear immediately after recovery in the postoperative period. The role played by doctors preserving most of the respiratory organs. When only the tumor is removed from the lung tissue, the patient recovers quickly. But if a lobe resection was performed, the standard of living deteriorates.
It is important to find out in time what pulmonary hamartoma is and undergo examinations and listen to the body. This way you can avoid complications.
Author: Evgeniya Leshenkova Therapist, pulmonologist
Treatment of the disease
Treatment of hamartoma is only surgical. The only exception is small hamartomas, up to 2.5 centimeters. In such cases, clinicians take a wait-and-see approach: the patient is under constant supervision by a pulmonologist, which can last for years.
In other situations, surgery is necessary. Indications for surgical intervention:
- single neoplasm larger than 2.5 centimeters;
- hamartoma growth;
- inability to eliminate symptoms with medication;
- the clinician’s doubts regarding the benign quality of the formation;
- strong mental worries about the presence of such a tumor in a person.
Surgery can be performed in several ways:
- segmental or marginal resection of the lung;
- desquamation of the tumor;
- removal of the affected pulmonary lobe;
- bronchotomy with node excision;
- fenestrated or circular resection of the bronchus;
- complete excision of the affected lung.
Scheme of lung resection
In some cases, removal can be done using minimally invasive methods:
- evaporation with high-energy laser;
- use of an electrocoagulation loop;
- cryodestruction;
- argon plasma coagulation.
The choice of medical procedure is influenced by the size and location of the tumor.
Treatment of hamartoma with folk remedies is not carried out; moreover, it is contraindicated, as it can provoke tumor growth.
Symptoms of the disease
Healthy lung and hamartoma
In most situations, pulmonary hamartoma has a long and asymptomatic course. The tumor is discovered completely by accident during a preventative X-ray or at an autopsy.
Several symptoms may indicate the development of such an anomaly, including:
- severe cough - in the initial stages of the disease it is unproductive, but the more the problem worsens, the more sputum is produced, which may have a mucous or purulent consistency;
- hemoptysis;
- shortness of breath that occurs after prolonged physical activity;
- wheezing when breathing;
- local discomfort in the chest area;
- signs of bronchitis and pneumonia.
Multiple hamartomas lead to the Carney triad, which can be combined with gastric leiomyoblastoma and paraganglioma. Neoplasms are fraught with the development of Cowden syndrome, when multiple benign formations form on internal organs, which often causes the development of the following types of cancer:
- mammary glands;
- digestive system;
- genitourinary organs;
- thyroid gland.